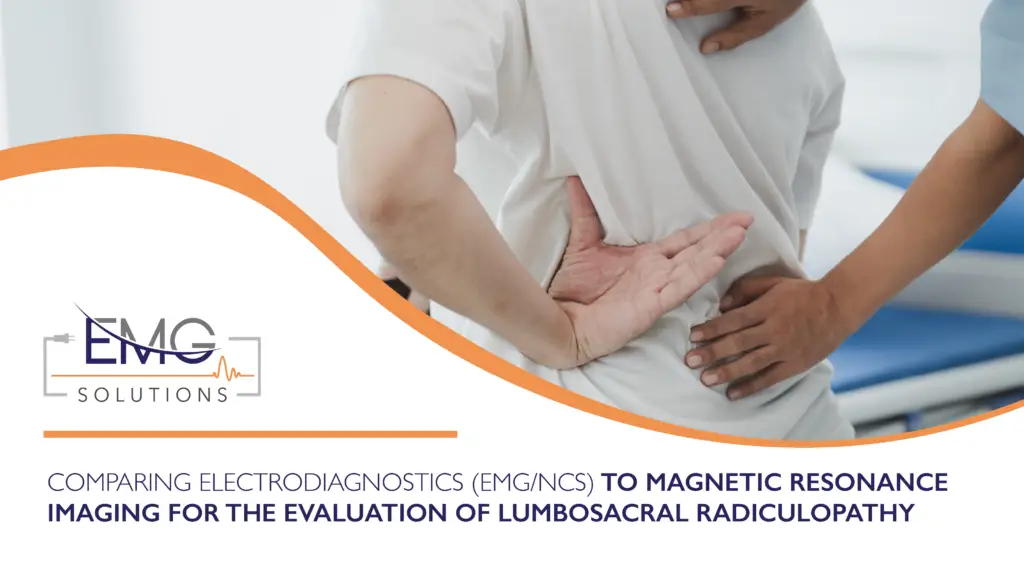
Low back pain and lumbar radiculopathy are common conditions affecting the general population. Low back pain has a prevalence of 10%-30%, and lumbar radiculopathy has a prevalence of 3%-5% [1].
Differentiating between low back pain and lumbar radiculopathy can be tricky, as low back pain is often used to describe a variety of conditions, from acute low back discomfort, referred pain, radicular pain, discogenic pain, mechanical low back pain, and radiculopathies [1,2]. Sorting through these various ailments can be tricky, as multiple muscles and structures can contribute to both low back pain and lower extremity pain (piriformis syndrome, psoas syndrome, greater trochanteric pain syndrome, and others), with a patient’s subjective report resembling lumbar radiculopathy [1].
Diagnostically, lumbosacral radicular pain is characterized by a radiating pain in one or more lumbar or sacral dermatomes. It may or may not be accompanied by other radicular irritation symptoms and/or symptoms of decreased function [3]. Due to the complexities and broad nature of the low back pain diagnosis, accurate
methods for identifying a true lumbar radiculopathy are an integral part of the diagnosis and treatment process. Magnetic Resonance Imaging (MRI) and Electrodiagnostic assessment (EDX) are two key tests that can aid in the assessment of nerve damage to allow for a definitive lumbar radiculopathy diagnosis.
Patients are often referred to physical therapy and may undergo a course of corticosteroids to treat the initial
inflammatory response, allowing the patient to participate in exercise that will facilitate return to function. However, if these conservative methods do not work, the patient may be a candidate for surgery.
MRI vs. Electrodiagnostic Testing for Lumbar Radiculopathy
In order to assess where the lesion is located and the severity of injury, physicians will often order MRI and electrodiagnostic testing before deciding to refer for surgical intervention. However, is one test better than the other, or should they be used together when building a differential diagnosis?
Mutaza et al. (2023) assessed 96 patients with complaints consistent with lumbar radiculopathy. They found that while MRI has been shown to be very sensitive (75% sensitivity) to disc herniations and anatomic abnormalities, it is not as specific (25% specificity), and not all findings are considered pathologic and may not be the cause of the patient’s current symptoms [4]. MRIs are primarily ordered to assess any physical compression of a nerve. It does not allow for an assessment of the function of a given nerve that has been compressed, or whether that compression is significant enough to cause the symptoms the patient is having.
Similarly, EDX is also very sensitive (75% sensitivity) to abnormalities of active and chronic nerve injuries, but is not very specific (25% specificity). The main difference between the two tests is that MRI has been shown to have a higher false negative (says it’s ok when it’s not), and EDX has a higher false positive (says there is damage when there is not) [4].
Yousif et al. (2020) examined 30 patients to assess any correlation between subjective symptoms and MRI and EDX findings. They found that 23 of the 30 patients examined had nerve root compression on MRI, with 20 patients (66%) having an abnormal physical exam and 3 (10% having no symptoms). Similarly, 22 of the 30 patients examined with NCS were found to have positive findings (prolonged H-Reflex, prolonged F-waves, as well as changes in amplitudes and/or conduction velocities in the tibial and fibular nerves). 17 (56%) of those tested with EDX had an abnormal physical exam, and 5 (17%) had a normal physical exam.
These findings agree with several previous and current studies [3-8]. The current consensus is that there is no statistically significant association between MRI and EDX findings with patient complaints individually, but they are both tools that should be used as supporting evidence when building a differential diagnosis. EDX appears to give a higher false positive for lumbar radiculopathy when compared to MRI [3,5] and can, in part, be explained by the different nature of each test. MRI assesses structural abnormalities that can affect the nerve, while EDX examines the physiological function of the nerve, with EMG being more sensitive to past injuries that may not be symptomatic at this time. Overall, EDX continues to be more specific and less sensitive when compared to MRI. In conclusion, both EDX and MRI should be used together to assess the presence of a lesion (MRI) and the severity of physiologic compromise (EDX) that may explain the patients’ current physical limitations/complaints.
Bibliography
- Bateman, Emma A., Christian D. Fortin, and Meiqi Guo. “Musculoskeletal mimics of lumbosacral radiculopathy.” Muscle & Nerve (2024).
- Kaito, Takashi, and Yu Yamato. “The essence of clinical practice guidelines for lumbar disc herniation, 2021: 3. Diagnosis.” Spine Surgery and Related Research 6.4 (2022): 325-328.
- Montaner-Cuello, Alberto, et al. “Comparison of Magnetic Resonance Imaging with Electrodiagnosis in the Evaluation of Clinical Suspicion of Lumbosacral Radiculopathy.” Diagnostics 14.12 (2024): 1258.
- Murtaza, Farhan, et al. “Correlation between Electrodiagnostic Study and Magnetic Resonance Imaging in Lumbar Radiculopathy Patients in a Tertiary Care Hospital.” Case Reports in Clinical Medicine 12.10 (2023): 363-370.
- Yousif, Safa, et al. “Correlation between findings in physical examination, magnetic resonance imaging, and nerve conduction studies in lumbosacral radiculopathy caused by lumbar intervertebral disc herniation.” Advances in Orthopedics 2020.1 (2020): 9719813.
- [10] T. D. Lauder, T. R. Dillingham, M. Andary et al., “Effect of history and exam in predicting electrodiagnostic outcome among patients with suspected lumbosacral radiculopathy,” American Journal of Physical Medicine & Rehabilitation, vol. 79, no. 1, pp. 60–68, 2000.
- [11] T. D. Lauder, “Physical examination signs, clinical symptoms, and their relationship to electrodiagnostic findings and the presence of radiculopathy,” Physical Medicine and Rehabilitation Clinics of North America, vol. 13, no. 3, pp. 451–467, 2002.
- [12] S. Nafissi, S. Niknam, and S. S. Hosseini, “Electrophysiological evaluation in lumbosacral radiculopathy,” Iranian Journal of Neurology, vol. 11, no. 3, pp. 83–86, 2012.
- [13] E. E. ˙ Inal, F. Eser, L. A. Aktekin, E. ¨ Oks¨ uz, and H. Bodur, “Comparison of clinical and electrophysiological findings in patients with suspected radiculopathies,” Journal of Back and Musculoskeletal Rehabilitation, vol. 26, no. 2, pp. 169–173, 2013.