Nerve conduction studies (NCS) and electromyography (ECS) help illuminate confusing neurologic cases and can pinpoint the origin of a problem. In this patient’s case it so happened to be from the suprascapular nerve.
Going to a bar with a friend or loved one does not always go wrong but for this 42-year old man things got messy when he was assaulted while getting a drink 3 years ago with his wife. After the traumatic ordeal he ended up bruised, bleeding, and with a broken right scapula. He was evaluated at the emergency room and sent on his way. It was not until months later that he noticed his right shoulder was feeling weaker. He attributed this to the injury and thought with time the pain would subside and his strength would return. But when he noticed the weakness progressively worsening, he began to worry.
A depiction of a person suffering from a shoulder problem. Image source: Wikimedia Commons.
Over the course of the next 3 years, he was treated for shoulder pain without any resolution of symptoms. It was at this time that a nerve conduction study and EMG were ordered to evaluate his right shoulder. Upon physical evaluation, two notable findings associated with the right shoulder were seen. A 3/5 manual muscle test grading with right side external rotation and muscular atrophy of the right infraspinatus muscle. All signs were pointing to a suprascapular nerve injury.
EMG and NCS tests confirmed the patient’s clinical findings. The signal recorded from the right supraspinatus muscle was comparable to the contralateral side and the signal recorded from the right infraspinatus muscle was only 40% as big as the left with a more dispersed waveform.

Figure 1: NCS traces from suprascapular-innervated muscles. Action potential amplitude is comparable from side to side when recording over the supraspinatus and dramatically decreased on the affected side when recording over the infraspinatus.
Needle EMG further illuminated these findings. Increased insertional activity, fibrillation potentials, positive sharp waves, along with reduced recruitment and 1-2 motor unit potentials in the infraspinatus muscle only, point to a long-standing nerve compromise at or around the curved free lateral border of the spine of the scapula (spinoglenoid notch).
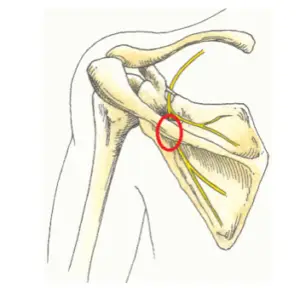
Suprascapular nerve around the scapula. Image source: Flickr Commons
While there are many reasons for shoulder pain and weakness, suprascapular nerve pathology has been noted as an overlooked cause.1 When evaluating a potential suprascapular nerve compromise the clinical exam is as important as are other diagnostic tests such as CT and MRI. However, the gold standard examination tool for the diagnosis of suprascapular nerve conditions are electromyography (EMG) and nerve conduction studies (NCS).1 In this patient’s situation not only was testing able to localize which nerve was affected but was also able to identify the exact location of compromise.
Whenever there is suspicion of nerve damage, early intervention often leads to the best outcomes, regardless of whether a conservative or surgical approach is taken.2 Electrodiagnostic testing is recommended to confirm suprascapular neuropathy and avoid the pitfall of misdiagnosis.2
Kyle J. Martinos PT, DPT, ECS
- Kostretzis L, Theodoroudis I, Boutsiadis A, Papadakis N, Papadopoulos P. Suprascapular Nerve Pathology: A Review of the Literature. Open Orthop J. 2017; 11:140-153. Published 2017 Feb 28. doi:10.2174/1874325001711010140
- Reece CL, Varacallo M, Susmarski A. Suprascapular Nerve Injury. [Updated 2020 Jul 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559151/