Foot drop—when you suddenly cannot lift the front of your foot—can be alarming. This condition often leads to an increased fall risk as well as an unusual gait pattern where one has to lift the knee higher to avoid dragging the foot, known as a “steppage gait.” But what exactly is happening when you lose the ability to lift your foot? Foot drop can stem from various conditions, with fibular (or peroneal) neuropathy and lumbar radiculopathy being two of the most common culprits. Here, we will dive into these possible causes, looking at their signs, symptoms, diagnostic tools, and ways to tell them apart.
Signs and Symptoms of Foot Drop
People with foot drop often experience:
- Difficulty lifting the front part of the foot (dorsiflexion)
- Altered gait patterns (typically a steppage or high-stepping gait) that help to clear the foot from the ground to prevent tripping
- Numbness, tingling, and/or pain along the top or side of the foot, around the outside of the lower leg, or along the outer knee
- Weakness in ankle dorsiflexion (ability to flex the foot upward) as well as weakness lifting the toes up (toe extension)
- Occasionally, weakness in bringing the foot out to the side (eversion).
Fibular (Peroneal) Neuropathy
Etiology and Risk Factors:
Fibular neuropathy is one of the most common causes of foot drop. It involves compression or damage to the fibular nerve, which wraps around the neck of the fibula, a bone located on the outer side of the knee. This nerve is particularly vulnerable because of its superficial location near the fibular head. Compression or damage here can impair the nerve’s ability to communicate signals to the muscles that lift the foot.
Common Risk Factors Include:
- Leg crossing or prolonged kneeling: These positions can compress the nerve against the fibula.
- Rapid weight loss: When someone loses a lot of weight over a short period of time, often seen after bariatric surgery or after starting weight-loss medications (such as Ozempic), a loss of protective fat around the nerve makes it more prone to injury.
- Prolonged hospitalizations: When laying in a hospital bed for a prolonged period of time, the legs may lay in an external rotation position where there is a lot of pressure on the outside of the knee – either by the bed rails or by the bed itself.
- Casting or splinting: Orthopedic casts or braces that press on the fibular head can also injure the nerve.
- Trauma: Direct injury to the outside of the knee or to the fibula, such as fractures or dislocations, can directly damage the nerve.
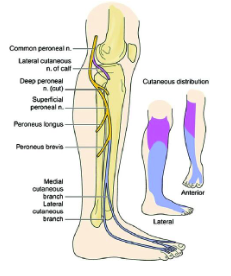
Signs and Symptoms Specific to Fibular Neuropathy:
Fibular neuropathy typically causes weakness in the muscles that allow the ankle to dorsiflex (lift the foot) but will only affect the other muscles that are innervated by the fibular nerve in the lower leg (below the knee). The muscles innervated by the tibial nerve (such as the gastrocnemius/soleus and posterior tibialis) will be spared, so the ability to stand on the tiptoes (plantarflexion) or pull the foot inwards (inversion) will be spared. Sensory symptoms (e.g., numbness or tingling) often occur along the top of the foot and the outer part of the lower leg/calf. Symptoms usually do not extend above the knee, which helps to differentiate it from other conditions that can cause foot drop.
Electrodiagnostic Findings (NCV/EMG):
Electrodiagnostic testing can help confirm fibular neuropathy. Nerve conduction studies (NCV) assess the speed and strength of electrical impulses through the nerve, and an EMG (electromyography) measures muscle response to these signals. In fibular neuropathy:
- NCV may show a slowed conduction velocity at the fibular head or a reduced response in the muscles innervated by the fibular nerve.
- The fibular nerve can be assessed by recording from different muscles in the lower leg, which helps to determine if the common fibular nerve has been affected or if the nerve damage has occurred after the common fibular nerve bifurcates into the superficial fibular and deep fibular nerves.
- EMG can reveal reduced muscle activation in the tibialis anterior and extensor digitorum longus, key muscles responsible for dorsiflexion and toe extension.
- If a fibular neuropathy is suspected, the NCV testing of the tibial nerve and the sural sensory nerve will be normal. EMG testing of muscles innervated by the tibial motor nerve will be normal.
- If a fibular neuropathy is suspected at the fibular head, other fibular motor muscles that are innervated above the knee will be normal. For example, abnormal findings in various fibular nerve muscles in the lower leg will be abnormal, but the biceps femoris – short head (which is innervated proximal to the fibular head) will be normal.
Lumbar Radiculopathy
Etiology and Risk Factors:
Lumbar radiculopathy involves irritation or compression of a nerve root in the lumbar spine. Foot drop often results from radiculopathy of the L4 or L5 nerve roots. These nerve roots form part of the sciatic nerve, which branches to control lower leg and foot movement. When the nerve root becomes irritated, inflamed, or compressed—often due to a herniated disc, spinal stenosis, or degenerative changes in the spine—it can impair signals to the muscles controlling dorsiflexion.
Common risk factors include:
- Age-related spinal degeneration: Conditions like osteoarthritis and spondylolisthesis become more common with age and can compress lumbar nerve roots.
- Heavy lifting or trauma: Activities that place sudden strain on the back, particularly when lifting or twisting, can increase risk.
- Sedentary lifestyle or poor posture: Weak core muscles and prolonged sitting may contribute to lumbar disc issues and, ultimately, radiculopathy.
Signs and Symptoms Specific to Lumbar Radiculopathy:
Lumbar radiculopathy often affects not only the foot, but also other areas supplied by the irritated nerve. Pain, tingling, or numbness may radiate from the lower back down through the buttock and thigh, occasionally reaching the calf or foot. Weakness may extend to muscles of the hip and thigh, and discomfort often increases with prolonged sitting, bending, or lifting.
Electrodiagnostic Findings (NCV/EMG):
In lumbar radiculopathy, NCV studies typically appear normal because the problem lies at the nerve root, not the peripheral nerves. EMG is more useful here:
- EMG might show signs of denervation (muscle dysfunction due to nerve issues) in the affected muscles, including the tibialis anterior if L5 is involved.
- A combination of findings in proximal and distal muscles along the path of the L4 and L5 nerve roots can indicate lumbar radiculopathy. These findings will include muscles that are supplied by the various peripheral nerves that can be traced back to the affected lumbar root level. For example, in an L4/L5 radiculopathy, EMG findings could be noted in muscles supplied by the fibular nerve (e.g., tibialis anterior, extensor hallucis longus), the tibial nerve (e.g., posterior tibialis), and even in some more proximal muscles supplied by the superior gluteal nerve (e.g., tensor fascia latae and gluteus medius).
- Although sensory changes may be felt in the lower leg, NCV testing of the sensory nerves will be normal since the sensory cell body (dorsal root ganglion) lies outside of the vertebral foramen and is not typically affected in a radiculopathy.
- In some cases, the NCV testing of the tibial and fibular motor nerves may show a reduced size of the compound motor action potential (CMAP), indicating that axonal loss is present.
- Also, with NCV testing, some of the long waves (e.g., tibial and fibular motor F-waves) may be prolonged or absent, indicating a slowing or loss of transmission of the nerves across the area of nerve compression in the spine.
Differentiating Fibular Neuropathy from Lumbar Radiculopathy
Understanding whether foot drop is caused by fibular neuropathy or lumbar radiculopathy is key to targeted treatment. Here are ways to tell them apart:
1.) Symptom Distribution:
- Fibular Neuropathy: Symptoms are usually restricted below the knee, specifically on the outer side of the knee, the outer lower leg/calf, and along the top of the foot.
- Lumbar Radiculopathy: Symptoms often radiate from the lower back down through the leg, possibly affecting areas above the knee. Think of this as the commonly described “sciatica” pattern that radiates from the back into the leg.
2.) Sensory Changes:
- Fibular Neuropathy: Numbness and tingling occur primarily on the top of the foot and outer calf.
- Lumbar Radiculopathy: Sensory changes often follow a path from the lower back down, possibly involving the thigh or buttock.
3.) NCV/EMG Results:
- Fibular Neuropathy: NCV shows decreased conduction at the fibular head. EMG shows dysfunction limited to distal muscles (below the knee). EMG will show normal fibular muscles that are innervated above the knee and will also include normal muscles that are supplied by other peripheral nerves (such as the Tibial nerve).
- Lumbar Radiculopathy: NCV is generally normal but may include reduced CMAPs when recorded from muscles supplied by nerve originating from the L4 or L5 nerve root levels; EMG reveals abnormalities in both proximal (thigh, hip) and distal (leg) muscles affected by the compressed nerve root (abnormalities will be noted in the muscles supplied by different peripheral nerves but all arising from the affected nerve root level).
4.) Positional Aggravation:
- Fibular Neuropathy: Crossing the legs, kneeling, or wearing tight casts or boots may worsen symptoms.
- Lumbar Radiculopathy: Prolonged sitting, bending, or lifting often exacerbates symptoms due to spinal compression.
Foot drop may seem like a simple issue on the surface, but it often reflects a complex interplay between muscles, nerves, and even spinal health. Fibular neuropathy and lumbar radiculopathy are two of the most common causes, each with its own unique origins, symptoms, and treatment pathways. While fibular neuropathy usually involves local compression of the nerve near the knee, lumbar radiculopathy points to a deeper issue in the lower spine, affecting nerve roots.
By recognizing the subtle differences in symptom patterns, such as where you feel numbness or what positions make symptoms worse, individuals and their healthcare providers can better understand which underlying issue might be at play. Diagnostic tools like NCV and EMG offer precise insight, helping to differentiate between these conditions and guiding effective treatment.
Whether the solution is as simple as avoiding leg-crossing or as involved as spinal decompression, knowing the cause of foot drop allows for more targeted interventions and a quicker path to recovery. So, while foot drop may seem like your foot’s refusal to cooperate, it’s often a signal of something deeper—and finding the root cause can make all the difference in regaining strength, stability, and confidence in every step.
Drayton Perkins, PT, DPT, ECS
Image 1: Fibular (Peroneal) Nerve – https://wikism.org/File:Distribution_of_the_fibular_common_superficial_and_deep_nerves.jpg